Our team of specialist solicitors regularly post stories and updates that are pertinent to their field of expertise. Find our latest blogs, campaigns and media mentions here.

We are passionate about improving the lives of all people who suffer serious injury. Read about the campaigns we have been working on.
Hear from our leading specialist solicitors and their guests, discussing the latest developments affecting those who have experienced serious injury.

In this episode, our Managing Partner Jonathan Wheeler chats to John Hyde, the Law Society Gazette’s Deputy News Editor. This is the second part of Jonathan and John’s…

In this episode, Ahmed Al-Nahhas, Partner and Head of our Military Claims team speaks to Caroline Paige MBE, veteran and founder of charity, Fighting With Pride.…

In this episode, Rhiannon Daniel, Partner in our Spinal Injury team speaks to Sucheta Iyengar, consultant obstetrician and gynaecologist about menopause in relation to Spinal…
Watch our dedicated specialist solicitors talk about their work and why we are passionate about delivering the best possible results to improve our clients’ quality of life.

For the second webinar in our Stoma and SCI series we were delighted to welcome Ant and Harry, members of the SCI (spinal cord injury)…

We were pleased to welcome Professor Anton Emmanuel to speak in our first of two webinars about stoma and spinal cord injury, hosted by Rhiannon…

Our team understands the life-changing impact of spinal injury. They only represent clients with spinal cord injuries, so they are true specialists in their field. …
Our expert team of specialist solicitors regularly post stories and updates about their work and areas of interest. Find our latest blogs here.

Bolt Burdon Kemp welcomes its first solicitor to qualify through the Level 7 SQE apprenticeship route. Connor Hawkins joined the firm in August 2022 as…

A convicted sex offender who was hired as a church caretaker has been sentenced for further sexual crimes against adolescent girls. Edward Hanbury abused young…
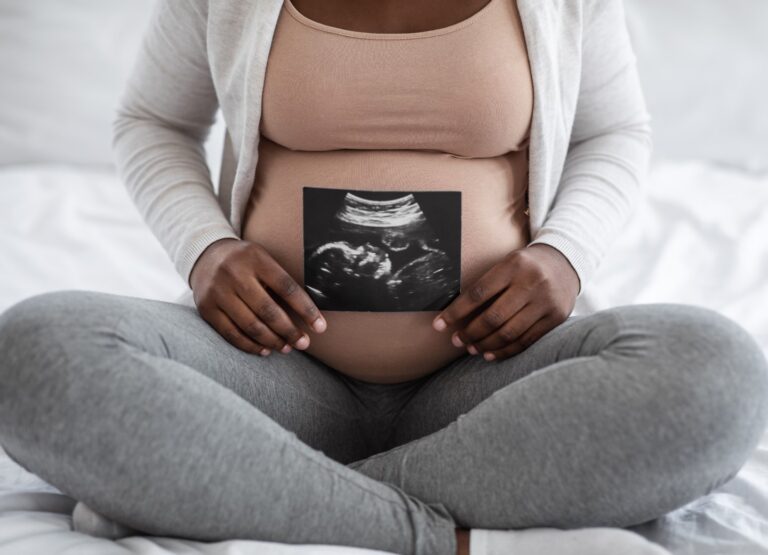
Wes Streeting’s announcement of a public inquiry into maternity services confirms what has been obvious for some time now – that maternity services nationwide are…
Our leading solicitors are regularly asked to comment on issues in the news, and share their expert insights. Find our latest media appearances here.
We regularly host and attend events for both the legal and charity communities. We support many incredible charities whose work helps improve the lives of the seriously injured. Here’s what’s coming up and where we’ve been.

The Brain Injury Team at Bolt Burdon Kemp is proudly working with Action for Recovery from Neurological Injury to hold a free online conference on stroke recovery…

Want to talk to one of our experienced lawyers? We can call when it suits you for a no-obligation, strictly confidential chat.
Your browser is out of date. Please update your browser.
This site (and many others) provides a limited experience on unsupported browsers and not all functionality will work correctly or look its best.